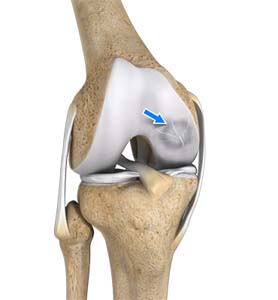
What is Osteochondral Defect of the Knee?
An osteochondral defect, also commonly known as osteochondritis dissecans, of the knee refers to a damage or injury to the smooth articular cartilage surrounding the knee joint and the bone underneath the cartilage. The degree of damage may range from a rupture of the cartilage to a slight crack of the bone to a piece of the bone breaking off within the joint. These pieces may vary in size and depth and may remain stable or unstable within the joint. These may occur from an acute traumatic injury to the knee or an underlying disorder of the bone. Osteochondral defect is more common among young athletes who actively take part in sports and most commonly affects the femoral condyles in the knee.
Anatomy
Each knee has two femoral condyles, the medial femoral condyle on the inside of the knee and the lateral femoral condyle on the outside of the knee. The two femoral condyles make up the rounded end of the femur (thigh bone). Osteochondral defects occur within the lateral aspect of the medial femoral condyle.
Causes of Osteochondral Defect of the Knee
The causes of an osteochondral defect of the knee are still unclear; however, some theories include deficient blood supply to the injured region, direct trauma, repetitive strain, or heredity.
Symptoms of Osteochondral Defect of the Knee
Some of the common symptoms associated with osteochondral defect of the knee include:
Pain
Tenderness
Swelling
Joint instability
Decreased mobility
Catching or locking sensation
Diagnosis of Osteochondral Defect of the Knee
Your doctor will physically examine the knee joint for instability and range of motion. if your doctor feels any abnormality during the examination, an X-ray may be ordered for further details. If a cartilage tear or other abnormality is difficult to see on an X-ray, a magnetic resonance imaging (MRI) or computed tomography (CT) scan may be ordered for confirmation and diagnosis of an osteochondral defect.
Treatment for Osteochondral Defect of the Knee
Your physician may recommend various treatments depending on the reports of diagnostic scans, age, severity, stability of the cartilage, and other factors.
Conservative treatment approaches such as the wait-and-watch approach, pain medications, and immobilization for 1-2 weeks are recommended if the condition is diagnosed at the early stages and the condition is mild. However, surgery is required if the condition is diagnosed at an advanced stage or is severe.
Surgery for osteochondral defect of the knee can be performed using the open or arthroscopic technique. Some of the surgical procedures include:
- Drilling: In this method, multiple small holes are drilled into the bone to allow the growth of new blood vessels in the defected area. This promotes blood flow into the defective area, initiating the healing response and formation of new cartilage cells.
- Open reduction internal fixation (ORIF): Open surgery is performed in cases where the defected area is difficult to reach with an arthroscope. Hence, an open incision may be required. In this procedure, an incision is made in front of the joint to allow your surgeon to view the joint and remove the loose bodies. Internal fixation involves fixing the fragments using internal fixators such as metal screws, pins, and wires.
- Bone grafting: It helps to fill the gap after the removal of the dead or necrotic bone. In this procedure, bone graft is placed on the damaged site. This procedure may be performed to repair the damaged area or replace the missing bone. Autograft (harvested from the same individual) or allograft (taken from the bone bank) may be required to help in the growth of a new bone.
- Osteochondral grafting: The procedure involves the transfer of healthy cartilage plugs from a non-weight-bearing area of the joint to the damaged area of the joint in a mosaic pattern. It allows the newly implanted bone and cartilage to grow in the defected area. Grafts may be taken from your own body (autograft), or from a donor or bone bank (allograft).
- Autologous chondrocyte implantation (ACI): In this procedure, healthy cartilage cells are harvested from your non-weight-bearing joint and cultured in the laboratory. The cultured cartilage tissue patch will be implanted into the defected area to promote the growth of new cartilage.
Related Topics:
- Knee Pain
- Knee Sprain
- ACL Tears
- Meniscal Tears
- Patellar Instability
- Chondromalacia Patella
- Jumper's Knee
- Kneecap Bursitis
- Baker's Cyst
- Iliotibial Band Syndrome
- Lateral Patellar Compression Syndrome
- Fractures of the Tibia
- Osteochondritis Dissecans of the Knee
- Pediatric ACL Tears
- Shin Splints
- Knee Injury
- Unstable Knee
- Goosefoot Bursitis of the Knee
- MCL Tears
- MCL Sprains
- Meniscal Injuries
- Fractures of the Patella
- Ligament Injuries
- Multiligament Knee Injuries
- Multiligament Instability
- Knee Arthritis
- PCL Injuries
- Chondral or Articular Cartilage Defects
- Patellofemoral Instability
- Patella Fracture
- Recurrent Patella Dislocation
- Quadriceps Tendon Rupture
- Patellar Tendon Rupture
- Lateral Meniscus Syndrome
- Tibial Eminence Spine Avulsion Fracture
- Posterolateral Instability
- Osteonecrosis of the Knee
- Knee Angular Deformities
- Osteochondral Defect of the Knee
- Medial Gastrocnemius Strain
- Articular Cartilage Injury
- Loose Bodies in the Knee
- Knee Fracture
- Knee Osteoarthritis
- Knee Sports Injuries
- Patellar Tendinitis
- Pediatric Tibial Tubercle Fractures
- Women and ACL Injuries
- Medial Meniscus Syndrome
- Adolescent Knee Problems
- Anterior Knee Pain
- Runner's Knee
- Osgood-Schlatter Disease
- Patellar Dislocation/Patellofemoral Dislocation
