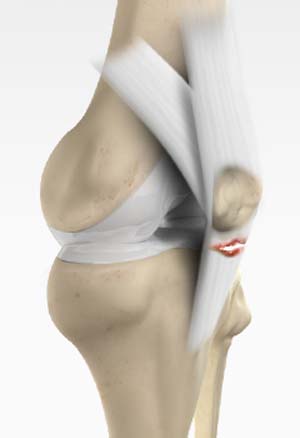
What is Patellar Tendon Rupture?
The patellar tendon works together with the quadriceps muscle and the quadriceps tendon to allow your knee to straighten out. Patella tendon rupture is the rupture of the tendon that connects the patella (kneecap) to the top portion of the tibia (shinbone).
Causes of Patellar Tendon Rupture
A patellar tendon tear most commonly occurs in middle-aged people who participate in sports that involve jumping and running. It can rupture due to a fall, direct blow to the knee or landing on your foot awkwardly from a jump. The other causes may include patellar tendonitis (inflammation of patellar tendon), diseases such as rheumatoid arthritis, diabetes mellitus, infection, and chronic renal failure. The use of medications such as steroids can cause increased muscle and tendon weakness.
Symptoms of Patellar Tendon Rupture
When the patellar tendon tears, the patella may lose its anchoring support on the tibia, as a result, when the quadriceps muscle contracts, the patella may move up into the thigh. You are unable to straighten your knee and upon standing, the knee buckles upon itself. In addition to this, you may have pain, swelling, tenderness, a tearing or popping sensation, bruising and cramping.
A patellar tendon tear can be a partial or complete tear.
- In a partial tear, some of the fibers in the tendon are torn, but the soft tissue is not damaged.
- In a complete tear, the soft tissues are disrupted into two pieces.
Diagnosis of Patellar Tendon Rupture
To identify a patellar tendon tear, your doctor will review your medical history and perform a physical examination of your knee. Some imaging tests, such as an X-ray or magnetic resonance imaging (MRI) scan may be ordered to confirm the diagnosis.
Treatment of Patellar Tendon Rupture
Patellar tendon ruptures can be treated by non-surgical and surgical methods.
Non-surgical Treatment of Patellar Tendon Rupture
Non-surgical treatment involves the use of braces or splints to immobilize the knee. Physical therapy may be recommended to restore the strength and increase the range of motion of the knee.
Surgical Treatment of Patellar Tendon Rupture
The goal of the surgery is to reattach the torn tendon to the kneecap and restore the normal function in the affected leg. Surgery is performed under regional or general anesthesia on an outpatient basis. An incision is made on the front of the knee to expose the ruptured tendon. Holes are made in the patella. Strong sutures are tied to the tendon and threaded through these holes. These sutures are tied in place to pull the torn edge of the tendon back to its normal position on the kneecap.
Severe damage can make the patellar tendon very short, and in such cases, reattachment will be difficult. Your surgeon may attach a tissue taken from a donor (allograft) to lengthen the tendon.
Postsurgical Care
Following surgery, a brace may be necessary to protect the healing tendon. Complete healing of the tendon will take about 6 months.
Risks and Complications of Surgical Treatment of PatellarTendon Rupture
As with all surgeries, surgery for patellar tendon rupture may be associated with certain risks and complications such as weakness and loss of motion. In some cases, the tendon that is re-attached may detach from the kneecap or tear. Other complications such as infection and blood clot may be observed.
Related Topics:
- Knee Pain
- Knee Sprain
- ACL Tears
- Meniscal Tears
- Patellar Instability
- Chondromalacia Patella
- Jumper's Knee
- Kneecap Bursitis
- Baker's Cyst
- Iliotibial Band Syndrome
- Lateral Patellar Compression Syndrome
- Fractures of the Tibia
- Osteochondritis Dissecans of the Knee
- Pediatric ACL Tears
- Shin Splints
- Knee Injury
- Unstable Knee
- Goosefoot Bursitis of the Knee
- MCL Tears
- MCL Sprains
- Meniscal Injuries
- Fractures of the Patella
- Ligament Injuries
- Multiligament Knee Injuries
- Multiligament Instability
- Knee Arthritis
- PCL Injuries
- Chondral or Articular Cartilage Defects
- Patellofemoral Instability
- Patella Fracture
- Recurrent Patella Dislocation
- Quadriceps Tendon Rupture
- Patellar Tendon Rupture
- Lateral Meniscus Syndrome
- Tibial Eminence Spine Avulsion Fracture
- Posterolateral Instability
- Osteonecrosis of the Knee
- Knee Angular Deformities
- Osteochondral Defect of the Knee
- Medial Gastrocnemius Strain
- Articular Cartilage Injury
- Loose Bodies in the Knee
- Knee Fracture
- Knee Osteoarthritis
- Knee Sports Injuries
- Patellar Tendinitis
- Pediatric Tibial Tubercle Fractures
- Women and ACL Injuries
- Medial Meniscus Syndrome
- Adolescent Knee Problems
- Anterior Knee Pain
- Runner's Knee
- Osgood-Schlatter Disease
- Patellar Dislocation/Patellofemoral Dislocation
