Patellar Tendon Rupture
Patella tendon rupture is the rupture of the tendon that connects the patella (kneecap) to the top portion of the tibia (shinbone). The patellar tendon works together with the quadriceps muscle and the quadriceps tendon to allow your knee to straighten out.
When the patellar tendon tears, the patella may lose its support; as a result, when the quadriceps muscle contracts, the patella may move up into the thigh. You are unable to straighten your knee and upon standing, the knee buckles upon itself. In addition to this, you may experience pain, swelling, tenderness, a tearing or popping sensation, bruising and cramping.
A patellar tendon tear can be a partial or a complete tear. In a partial tear, some of the fibers in the tendon are torn, but the soft tissue is not damaged. In a complete tear, the soft tissues are disrupted into two pieces.
Treatment of Patellar Tendon Rupture
Patellar tendon rupture can be treated by non-surgical and surgical methods. Non-surgical treatment involves the use of braces or splints to immobilize the knee. Physical therapy may be recommended to restore the strength and increase the range of motion of the knee.
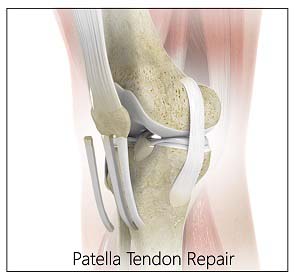
Patellar Tendon Repair
The goal of the surgery is to reattach the torn tendon to the kneecap and to restore normal function in the affected leg. The procedure is performed under regional or general anesthesia and an incision is made on the front of the knee to expose the tendon rupture. Holes are made in the patella, strong sutures are tied to the tendon and then threaded through these holes. These sutures pull the torn edge of the tendon back to its normal position on the kneecap.
Severe damage can make the patellar tendon very short, and in such cases, reattachment will be difficult. Your surgeon may attach a tissue taken from a donor (allograft) to lengthen the tendon.
Recovery following Patellar Tendon Repair
Following surgery, a brace may be needed to protect the healing tendon. Complete healing of the tendon will take about 6 months.
Risks and Complications of Patellar Tendon Repair
As with all surgeries, patella tendon repair may be associated with certain risks and complications. Complications after the repair may include infection, blood clot, weakness, loss of motion, detachment from the kneecap or retears.
Related Topics:
- Knee Arthroscopy
- ACL Reconstruction
- Multiligament Reconstruction of the Knee
- Meniscal Surgery
- Cartilage Restoration
- Orthobiologics
- ACL Reconstruction with Patellar Tendon
- Partial Arthroscopic Meniscectomy
- Saucerization
- Intraarticluar Knee Injection
- Knee Fracture Surgery
- Arthroscopic Debridement
- LPFL Reconstruction
- Tibial Derotational Osteotomy
- Failed Meniscus Repair
- Meniscal Transplantation
- Meniscectomy
- Mosaicplasty
- Posterolateral Corner Reconstruction
- Prior Meniscectomy
- Quadriceps Tendon Repair
- Tibial Eminence Fracture
- Trochleoplasty
- ORIF of the Knee Fracture
- Chondroplasty
- Distal Femoral Osteotomy
- Hamstring Autograft
- Hamstring Allograft
- Viscosupplementation
- Physical Therapy for Knee
- Knee Osteoarthritis
- High Tibial Osteotomy
- Tibial Tubercle Osteotomy
- Patellar Tendon Repair
- Robotic Assisted Partial Knee Surgery
- Distal Realignment Procedures
- PCL Reconstruction
- LCL Reconstruction
- MCL Reconstruction
- Cartilage Replacement
- Bicompartmental Knee Resurfacing
- Autologous Chondrocyte Implantation
- Subchondroplasty
- Partial Meniscectomy
- Transphyseal Surgery
- Partial Transphyseal Surgery
- Medial Patellofemoral Ligament Reconstruction
- ACL Reconstruction Procedure with Hamstring Tendon
- Physeal Sparing Surgery (Anderson's Technique)
- Physeal Sparing Surgery (Micheli-KocherTechnique)
- Combined Hyaluronic Therapy for the Knee
- Matrix Induced Autologous Chondrocyte Implantation (MACI)
- Failed Anterior Cruciate Ligament (ACL) Reconstruction
- Physeal Sparing Reconstruction of the Anterior Cruciate Ligament
- Bone-Patellar Tendon-Bone (BPTB) Autograft
- Bone-Patellar Tendon-Bone (BPTB) Allograft
- Pharmacological Interventions for Knee Injuries
- Arthroscopic Reconstruction of the Knee for Ligament Injuries
