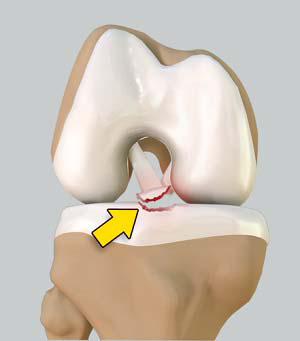
The tibia or shin bone is a major bone of the leg which connects the knee to the ankle. A fracture or break in the upper part of the tibia is known as a proximal tibial fracture and commonly occurs just below the knee joint.
The knee joint is the largest weight-bearing joint of the body, where the lower end of the femur or thigh bone articulates with the tibial plateau. The upper fourth of the tibia constitutes the proximal part and is composed of cancellous bone. By nature, cancellous bone easily undergoes compression and depression, following an injury. So the proximal tibia is at high risk for injury. A fracture in the proximal tibia may or may not affect the knee joint but the surrounding soft tissues, as well as the nerve and blood vessels, may be affected. A fracture in the top of the shin bone or tibial plateau, involving the articular cartilage surface of the knee joint, may develop chronic arthritis.
Causes
A fracture of the proximal tibia may be caused by stress or trauma or secondary to weakening of the bone due to cancer or infection. High energy injuries such as a fall from a height, sports-related trauma or motor vehicle accidents may be responsible for fracture in young adults. Sometimes even low energy injuries such as falling from a standing position may result in a fracture of the proximal tibia in elderly individuals.
Symptoms
The symptoms of proximal tibia fracture include painful weight-bearing movements, tenseness around the knee, limitation of movement and deformity around the knee. In some individuals, impairment of blood supply secondary to the fracture may result in a pale or cool foot. Patients may also experience numbness or feelings of ‘pins and needles’ in the foot as a result of associated nerve injury.
Diagnosis
The diagnosis of a proximal tibia fracture is based on the medical history including history of any previous injuries, complete physical examination and imaging studies. The physician will evaluate soft tissue around the joint to identify any signs of nerve or blood vessel injury. Multiple X-rays and other imaging studies such as CT and MRI scans may be used to identify the location and severity of the fracture.
Treatment
The management of the fracture is based on the severity of the fracture, the medical condition of the patient and the patient’s lifestyle.
Non-surgical treatment
Non-surgical treatment comprises immobilizing the fracture site with the help of casts or braces to prevent weight-bearing and to help the healing process. X-rays are taken at regular intervals to assess the healing process. Weight-bearing and movement are initiated gradually, depending on the nature of the injury and the condition of the patient.
Surgical treatment
Surgical treatment is considered to maintain alignment of the fractured bone. External or internal fixators may be used to align the fractured bone segments. If the fracture does not involve the knee joint, rods and plates can be used to stabilize the fracture. For a fracture involving the knee joint, a bone graft may be required to prevent the knee joint from collapsing. An external fixator is used when the surrounding soft tissue is severely damaged, as the use of plate and screw may be harmful.
Rehabilitation
As the proximal tibial fracture usually involves the weight-bearing joint it may cause long term problems such as loss of knee motion or instability and long term arthritis. Hence a rehabilitation program is initiated along with the treatment comprising of instructions on weight-bearing, knee movements, and the use of external devices such as braces.
Related Topics:
- Knee Arthroscopy
- ACL Reconstruction
- Multiligament Reconstruction of the Knee
- Meniscal Surgery
- Cartilage Restoration
- Orthobiologics
- ACL Reconstruction with Patellar Tendon
- Partial Arthroscopic Meniscectomy
- Saucerization
- Intraarticluar Knee Injection
- Knee Fracture Surgery
- Arthroscopic Debridement
- LPFL Reconstruction
- Tibial Derotational Osteotomy
- Failed Meniscus Repair
- Meniscal Transplantation
- Meniscectomy
- Mosaicplasty
- Posterolateral Corner Reconstruction
- Prior Meniscectomy
- Quadriceps Tendon Repair
- Tibial Eminence Fracture
- Trochleoplasty
- ORIF of the Knee Fracture
- Chondroplasty
- Distal Femoral Osteotomy
- Hamstring Autograft
- Hamstring Allograft
- Viscosupplementation
- Physical Therapy for Knee
- Knee Osteoarthritis
- High Tibial Osteotomy
- Tibial Tubercle Osteotomy
- Patellar Tendon Repair
- Robotic Assisted Partial Knee Surgery
- Distal Realignment Procedures
- PCL Reconstruction
- LCL Reconstruction
- MCL Reconstruction
- Cartilage Replacement
- Bicompartmental Knee Resurfacing
- Autologous Chondrocyte Implantation
- Subchondroplasty
- Partial Meniscectomy
- Transphyseal Surgery
- Partial Transphyseal Surgery
- Medial Patellofemoral Ligament Reconstruction
- ACL Reconstruction Procedure with Hamstring Tendon
- Physeal Sparing Surgery (Anderson's Technique)
- Physeal Sparing Surgery (Micheli-KocherTechnique)
- Combined Hyaluronic Therapy for the Knee
- Matrix Induced Autologous Chondrocyte Implantation (MACI)
- Failed Anterior Cruciate Ligament (ACL) Reconstruction
- Physeal Sparing Reconstruction of the Anterior Cruciate Ligament
- Bone-Patellar Tendon-Bone (BPTB) Autograft
- Bone-Patellar Tendon-Bone (BPTB) Allograft
- Pharmacological Interventions for Knee Injuries
- Arthroscopic Reconstruction of the Knee for Ligament Injuries
