What is Tibial Derotational Osteotomy?
Tibial derotational osteotomy is a surgical procedure employed to treat rotational deformities of the tibia, such as tibial torsion. This is a condition characterized by twisting of the tibial bone of the lower leg, causing malalignment of the knee and ankle with an appearance of an inward or outward turning of the feet.
A tibial derotational osteotomy necessitates the surgeon to incise the bone, turn it appropriately to improve the alignment, and secure the bones in that position with metal hardware while they heal.
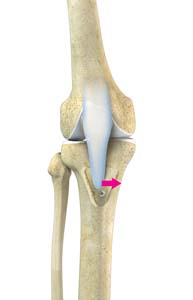
Anatomy of the Knee
The knee is made up of the femur (thighbone), the tibia (shinbone), and the patella (kneecap). The lower end of the thighbone meets the upper end of the shinbone at the knee joint. A small bone called the patella (kneecap) rests on a groove on the front side of the femoral end. A bone of the lower leg (fibula) forms a joint with the shinbone. The bones are held together by protective tissues, ligaments, tendons, and muscles. Synovial fluid within the joint aids in smooth movement of the bones over one another. The meniscus, a soft crescent-shaped cartilage between the femur and tibia, serves as a cushion and helps absorb shock during motion.
Indications for Tibial Derotational Osteotomy
Some of the common indications for tibial derotational osteotomy include:
- Tibial torsion
- Bowed legs
- Inward toeing
- Patellofemoral instability
- Rotational tibial deformities due to myelodysplasia and cerebral palsy
- Tibialis spasticity (extreme stiffness or tightness of the muscles that interfere with normal movement)
- Failure of conservative treatment
Preparation for Tibial Derotational Osteotomy
Preoperative preparation for tibial derotational osteotomy will involve the following steps:
- A thorough examination of the patient is performed by your doctor to check for any medical issues that need to be addressed prior to surgery.
- Depending on the patient’s medical history, social history, and age, routine blood work and imaging may be ordered for safely conducting surgery.
- Information regarding any allergies to medications, anesthesia, or latex is obtained.
- Information is also obtained on any medications, vitamins, or supplements being taken by the individual.
- The patient should refrain from medications or supplements such as blood thinners, aspirin, or anti-inflammatory medicines for a week or two prior to surgery.
- You should refrain from alcohol or tobacco at least 24 hours prior to surgery.
- You should not consume any solids or liquids at least 8 hours prior to surgery.
- Arrange for someone to drive you home as you will not be able to drive yourself post surgery.
- A written consent will be obtained after the surgical process has been explained in detail.
Procedure for Tibial Derotational Osteotomy
The main objective of the procedure is to correct in-toeing or out-toeing while walking due to rotational deformities of the tibia. In general, the procedure involves the following steps:
- A general or regional anesthesia is administered.
- An incision is made over the lower leg.
- Your surgeon performs an osteotomy (surgical cut of the bone) of the tibia and fibula, normally above the ankle.
- Your surgeon then turns or rotates the tibia bone accordingly to achieve a proper alignment.
- Metal hardware, such as pins are placed in the bone just below the knee to hold the bones in position.
- Pins will be removed at a later date after appropriate healing is confirmed.
- The surgical incisions are closed in layers and a sterile dressing is applied.
- A cast will be placed beginning at the pin and covering the entire leg and foot which holds the legs from moving while the new bone develops.
Postoperative Care Instructions and Recovery
In general, postoperative care instructions and recovery for tibial derotational osteotomy involves the following:
- The patient will be transferred to the recovery area to be monitored until awake from the anesthesia.
- A staff nurse will monitor blood oxygen levels and other vital signs as the patient recovers.
- Once awake, the patient may notice pain and discomfort. Pain relievers and muscle relaxants will be provided for comfort.
- Do not weight bear for at least 24 hours. You are encouraged to walk with assistance as frequently as possible to prevent blood clots.
- You are advised to keep your leg elevated while resting to prevent swelling and pain.
- Medications will also be prescribed as needed for symptoms associated with anesthesia, such as vomiting and nausea.
- Keep your cast clean and dry. Instructions on cast care and bathing will be provided. The patient may have to stay in the cast for 4 to 6 weeks.
- Eating a healthy diet rich in vitamin D is strongly advised to promote healing and a faster recovery.
- Refrain from strenuous activities or lifting heavy objects for a month or two. Gradual increase in activities over a period of time is recommended.
- An individualized physical therapy protocol is designed to strengthen muscles and restore muscle function.
- You will be able to return to your normal weight-bearing activities in 4 to 6 weeks, however, return to sports may take 3 to 6 months.
- A follow-up appointment for X-rays and pin removal 4 weeks after surgery will be scheduled as well as to monitor your overall progress.
Risks and Complications
Tibial derotational osteotomy is a relatively safe procedure; however, as with any surgery, there are risks and complications that could occur, such as:
- Infection
- Damage to adjacent soft tissue structures
- Deep vein thrombosis (DVT)
- Anesthetic complications
- Failure of metal hardware
- Persistence of pain and nonunion
- Inability to achieve complete correction
Related Topics:
- Knee Arthroscopy
- ACL Reconstruction
- Multiligament Reconstruction of the Knee
- Meniscal Surgery
- Cartilage Restoration
- Orthobiologics
- ACL Reconstruction with Patellar Tendon
- Partial Arthroscopic Meniscectomy
- Saucerization
- Intraarticluar Knee Injection
- Knee Fracture Surgery
- Arthroscopic Debridement
- LPFL Reconstruction
- Tibial Derotational Osteotomy
- Failed Meniscus Repair
- Meniscal Transplantation
- Meniscectomy
- Mosaicplasty
- Posterolateral Corner Reconstruction
- Prior Meniscectomy
- Quadriceps Tendon Repair
- Tibial Eminence Fracture
- Trochleoplasty
- ORIF of the Knee Fracture
- Chondroplasty
- Distal Femoral Osteotomy
- Hamstring Autograft
- Hamstring Allograft
- Viscosupplementation
- Physical Therapy for Knee
- Knee Osteoarthritis
- High Tibial Osteotomy
- Tibial Tubercle Osteotomy
- Patellar Tendon Repair
- Robotic Assisted Partial Knee Surgery
- Distal Realignment Procedures
- PCL Reconstruction
- LCL Reconstruction
- MCL Reconstruction
- Cartilage Replacement
- Bicompartmental Knee Resurfacing
- Autologous Chondrocyte Implantation
- Subchondroplasty
- Partial Meniscectomy
- Transphyseal Surgery
- Partial Transphyseal Surgery
- Medial Patellofemoral Ligament Reconstruction
- ACL Reconstruction Procedure with Hamstring Tendon
- Physeal Sparing Surgery (Anderson's Technique)
- Physeal Sparing Surgery (Micheli-KocherTechnique)
- Combined Hyaluronic Therapy for the Knee
- Matrix Induced Autologous Chondrocyte Implantation (MACI)
- Failed Anterior Cruciate Ligament (ACL) Reconstruction
- Physeal Sparing Reconstruction of the Anterior Cruciate Ligament
- Bone-Patellar Tendon-Bone (BPTB) Autograft
- Bone-Patellar Tendon-Bone (BPTB) Allograft
- Pharmacological Interventions for Knee Injuries
- Arthroscopic Reconstruction of the Knee for Ligament Injuries
